Bloating, cravings, depression, breast tenderness … ugh. If you or your partner experience these symptoms in the days or weeks leading up to menstruation, you’re not alone. Premenstrual syndrome (PMS) affects up to 80% of women, and up to 20% of women report severe symptoms that significantly disrupt life. A subset of these women have symptoms so debilitating that they’ve been given a new diagnosis – premenstrual dysphoric disorder (PMDD).
Drug companies have hopped on board (with decent intentions) to help women who suffer from PMS. To treat PMS and PMDD, conventional practitioners often prescribe birth control pills, anti-inflammatories, diuretics and even depression meds like Prozac (which is given a special name, Sarafem, when used for PMDD). And while these drugs may be appropriate for some women, they carry with them a host of disappointing side effects like gut disruption, libido changes, and anxiety. No thanks!
I like to think about health from an evolutionary perspective, and I find it hard to believe that nature intended for half of the human population to suffer physically for days or weeks out of every month. Especially for something so intricately related to the sacred reproductive cycle. I doubt that our ancestors sat around for the week before their period putting hot stones on their bellies and groaning about their tender breasts. Is some hormonal symptomatology normal before we menstruate? Yes. But should it knock us down and take us out of our lives? No. Our society leads us to believe that PMS is a part of life that we just have to suffer from. I’m here to tell you that that is not true. You have the power to balance your hormones and skate through your cycle with a smile. Don’t believe me? Read on.
What Causes PMS?
So what causes PMS in the first place? We aren’t completely sure, though many theories exist. An understanding of the normal female menstrual cycle will help as we explore several of these theories.
A normal 25-32 day cycle is full of healthy fluctuations in hormone levels. At the beginning of each cycle, estrogen is secreted by a developing follicle in the ovary. When estrogen levels peak, a hormone called lutenizing hormone rises, stimulating ovulation – or the release of the mature egg from the follicle. Estrogen levels initially drop with ovulation, then they slowly climb again. At the same time, the sac that’s left behind after ovulation becomes a progesterone-secreting powerhouse, and we have a beautiful, harmonious progesterone increase to balance out the rising estrogen levels. Progesterone is a calming, grounding hormone, which is why we often feel really great for the week or so post-ovulation.
The interplay between estrogen and progesterone is super important. For many women, especially women with PMS, this balance is thrown off. Stress, nutrient deficiencies, and inconsistent or absent ovulation can cause progesterone levels to be lower than normal. This phenomenon, called “estrogen dominance”, can result in symptoms of estrogen excess – mood changes, tender breasts, and bloating.
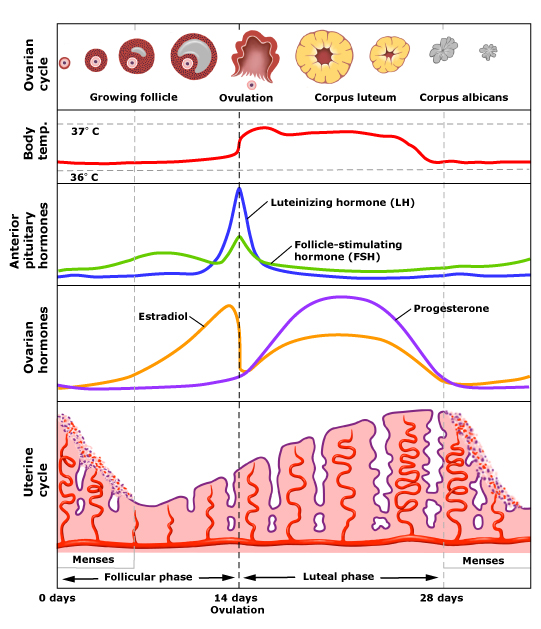
As you can see in the graphic, right before menses begin, there is a sudden and dramatic drop in both estrogen and progesterone levels. This hormone withdrawal is also believed to contribute to PMS symptoms. Some women are more sensitive to these delicate hormonal changes than others. There may be a genetic component as well, especially in women with PMDD (https://www.ncbi.nlm.nih.gov/pubmed?term=20172536).
Neurotransmitters also play an important role in PMS and PMDD. Women with PMS and PMDD tend to have lower levels of serotonin in their luteal phases (the weeks leading up to menstruation), and we think that this is related to hormonal impacts on the serotonin system (https://www.ncbi.nlm.nih.gov/pubmed?term=3627623). Similarly, low levels of vitamin B6, vitamin D, calcium and magnesium have been found in women with PMS, so there’s a role for nutrient deficiencies in this condition (https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4667262/)
Despite these hypotheses and the studies done to support them, we still aren’t 100% sure what causes PMS. There are likely multiple factors – genetics, hormones, neurotransmitters, nutritional deficiencies, and lifestyle. In integrative and functional medicine, we address symptoms and conditions from the ground up, focusing on whole-body health. This means initiating lifestyle changes, addressing nutrition, and balancing hormones. While this may take more time and effort than simply popping a Sarafem or Motrin, these changes promote lifelong health improvement, and a permanent solution (rather than a band-aid) for your monthly symptoms.
Here’s my root-cause resolution prescription for PMS and PMDD.
Root cause #1: Having a Sedentary Lifestyle
Studies suggest that sedentary women have a higher incidence of PMS than active women. These women tend to consume more calories around their period as well, which may contribute to further PMS symptoms such as bloating and blood sugar spikes. (http://lifescienceglobal.com/pms/index.php/jnt/article/view/4359)
Root cause resolution:
Aim for 30-60 minutes of movement 3-5 times per week, but especially during the days leading up to your period. Aerobic exercise like jogging, biking, interval training, and kickboxing can be especially helpful. So can weight training. Consider a combination of these. (https://www.ncbi.nlm.nih.gov/pubmed?term=8463989)
Root cause #2: Dietary Factors
An inflammatory diet full of processed foods, refined carbohydrates, conventional dairy, and sugar can contribute to PMS symptoms including anxiety and bloating. Many women crave high salt, high sugar, and high fat foods before their periods, and this can cause blood sugar dysregulation and make symptoms even worse.
Root cause resolution:
Eliminate sugar, processed foods, refined carbohydrates like bread, white rice, pasta, and all dairy from your diet for several cycles. Dairy is full of hormones that can impact our hormonal milieu, and many women are reactive to dairy. Removing it can be a game-changer for hormonal imbalances. Focus on lots of colorful vegetables, especially green leafy veggies which provide fiber and folate, a B vitamin that is important for mood. Eat protein with every meal, and include healthy fats such as nuts, seeds, olive oil, and avocados. Choose whole grains like quinoa, buckwheat, millet, and teff which provide extra fiber and B vitamins. Be especially mindful of your diet leading up to your period. Keep your blood sugar balanced by eating at least every 3-4 hours. If you have the urge to splurge, choose something healthy like a few squares of high-quality dark chocolate, or a spoonful of almond butter with some dark chocolate chips. You may find that eating a more balanced, healthy diet eliminates your cravings for “period foods” altogether!
Root cause #3: Detoxification Problems
Our bodies treat hormones the same way that they treat toxins – they get manipulated, neutralized, and eliminated once they’ve been used. However, if our garbage disposal system is backed up (i.e. if we are constipated or lacking the right nutrients to support the liver’s detox pathways), hormones can be reabsorbed into the bloodstream, leading to high levels of hormones like estrogen, and contributing to PMS.
Root cause resolution:
If you aren’t having a daily bowel movement, it’s time to start! Increase the fiber in your diet by aiming for 6-8 servings of vegetables every day, and drinking plenty of water. Boost your fiber intake by adding 1-2 tablespoons of ground flax seeds to your morning smoothie. If dietary changes aren’t enough to get things moving, add 300mg of magnesium citrate, at bedtime. This dose can be titrated over time to 600mg and should help to produce an easy-to-pass daily bowel movement.
Eat more cruciferous vegetables. Crucifers like cauliflower, kale, broccoli, Brussels sprouts, bok choy, and cabbage contain high levels of a compound called DIM which is important for the healthy detoxification of estrogens. (https://www.ncbi.nlm.nih.gov/pubmed/9539190) These veggies also provide lots of fiber, vitamins, and minerals. Eat the whole veggie – there’s lots of nutrition in broccoli stems, for example, so don’t just nibble the crowns!
Decrease alcohol. Studies have shown that women who drink more alcohol report worse PMS symptoms. (https://bmjopen.bmj.com/content/8/3/e019490.abstract) Alcohol interferes with the liver’s ability to detoxify hormones, which can lead to slower elimination of hormones, or hormone reabsorption which can increase hormone levels and contribute to hormonal symptoms.
Root cause #4: Nutritional Deficiencies
Women with PMS have been found to have lower levels of magnesium, vitamin D, calcium, and vitamin B6 when compared to women without PMS (https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4667262/)
Root cause resolution:
Food should always be our go-to source for nutrients. Eating a well-rounded diet that is full of real, whole foods including lots of veggies, fruits, proteins, and healthy fats ideally gives us what we need. Sometimes we need a little extra support due to our depleted food supply, falling short with our diets, or having underlying deficiencies from other factors. Women with PMS may benefit from targeted supplementation of the following nutrients that have been studied to improve PMS symptoms:
For details about recommended doses and formulations, see my Root Cause Rez Toolkit download at the end of this article!
Root cause #5: Stress
An often-cited 2010 study of 259 women found that women who had higher perceived stress early in their cycle went on to report more PMS symptoms, and this held true over subsequent cycles. (https://www.liebertpub.com/doi/abs/10.1089/jwh.2009.1717)
Root cause resolution:
Self-care is important for your mind, body – and hormones! Implement a stress-reducing practice that you can put into place when the going gets tough. Carve out some time every day for breathing and relaxing. If you are in a relationship, job, or social situation that is causing you stress, consider an exit strategy.
For a handy printable summary of these recommendations, including suggested supplement doses and additional tips, click here to download my PMS Root Cause Rez Toolkit!
As with any medical concern, consult your medical provider if you’re having severe symptoms, especially severe mood swings, significant cramps, or heavy menstrual bleeding during your periods. These recommendations are meant to be a guide, but you should always consult with a professional before starting any medical protocol.
Buying supplements
I’ve put together a PMS-busting supplement bundle at aswan.metagenics.com. Search for “PMS Bundle” or click here for the direct link. Use promo code HORMONE20 to save 20%!
You can also use Fullscript, my online supplement dispensary, to access high quality supplements at a discounted price. Click here to make your account or login. Then search for the PMS section in “My Favorites” to find direct links to the products mentioned in this toolkit.



